AARP study: S.C. nursing home COVID-19 infection rate worst in the nation
Staff Report //March 15, 2021//
AARP study: S.C. nursing home COVID-19 infection rate worst in the nation
Staff Report //March 15, 2021//
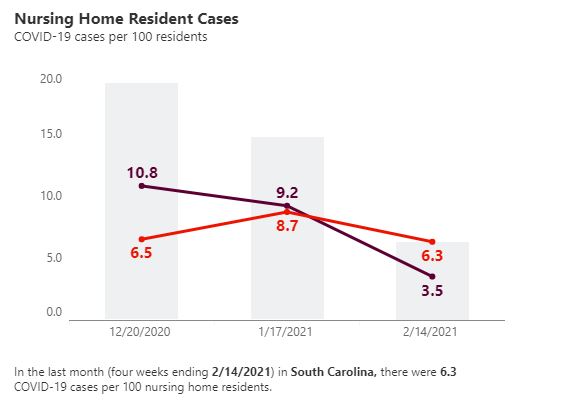
 South Carolina’s nursing homes still have the highest resident COVID-19 infection rates of any state with 6.3 residents out of every 100 infected by the virus from Jan. 18 to Feb. 14, according to a recent AARP report, despite a dip in staff and resident infections.
South Carolina’s nursing homes still have the highest resident COVID-19 infection rates of any state with 6.3 residents out of every 100 infected by the virus from Jan. 18 to Feb. 14, according to a recent AARP report, despite a dip in staff and resident infections.
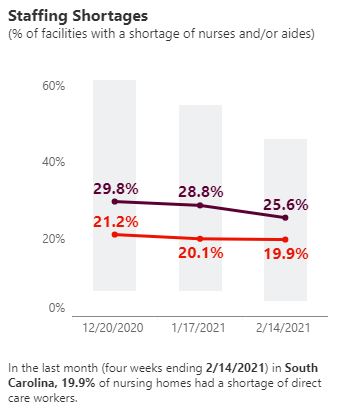
 Staffing shortages also continue to leave about 20%, or one out of every five, of the state’s nursing facilities in a lurch, according to the report.
Staffing shortages also continue to leave about 20%, or one out of every five, of the state’s nursing facilities in a lurch, according to the report.
"One year into the coronavirus pandemic, we continue to see disgracefully high numbers of cases and deaths in South Carolina nursing homes and long-term care facilities," Teresa Arnold, AARP South Carolina state director, said in a news release. "The vaccine rollout gives us hope, but we should not lose sight of the chronic, ongoing problems in our long-term care system that were exposed by COVID."
The study showed that COVID-19 deaths in nursing homes doubled over the eight-week span with 1.58 residents per every 100 losing their lives to the virus. Four other states had higher death rates: Georgia, North Carolina, Pennsylvania and Virginia.
AARP responded with a letter to the Centers for Medicare and Medicaid Services requesting the need to consider the level of vaccinations in facilities and the adherence to COVID-19 infection prevention principles.
 “As we enter a new phase of this pandemic with the ongoing rollout of vaccines and growing knowledge about public health needs — including the safety, mental health and social well-being of nursing home residents – it is vital that these vulnerable seniors are able to safely visit with their loved ones,” Nancy LeaMond, executive vice president and chief advocacy and engagement officer of AARP, said in a statement.
“As we enter a new phase of this pandemic with the ongoing rollout of vaccines and growing knowledge about public health needs — including the safety, mental health and social well-being of nursing home residents – it is vital that these vulnerable seniors are able to safely visit with their loved ones,” Nancy LeaMond, executive vice president and chief advocacy and engagement officer of AARP, said in a statement.
Staffing shortages continue to plague nursing homes across the nation. About 15,600 facilities reported the average annual turnover for staff had reached 128%, according to a study published this month. Some facilities had staff turnover rates higher than 300%, a problem compounded by the fact that one out of every 10 facilities did not have a one-week supply of personal protective equipment on hand in the last month.